
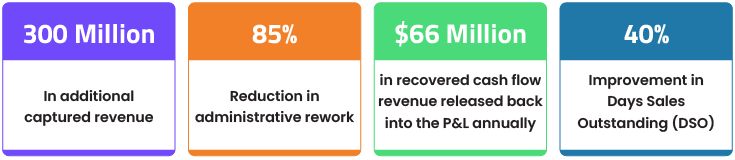
Forecasted Operational & Strategic Outcomes
One of the largest member-owned health insurers in North America. They serve 30 million members across a vast national network that includes hundreds of thousands of providers and more than 10,000 hospitals.
Managing 189,000 monthly transactions across 300 decentralized facilities through manual, daily processes created a systemic crisis where our clinical leaders were often performing as data entry clerks.
This administrative fragmentation resulted in a “black hole” of visibility, where regional variations in documentation led to revenue leakage and an unsustainable operational burden.
Lateetud implemented a centralized Charge Reconciliation Platform built on SharePoint and Microsoft 365 that automated the intake, review, and tracking of billing charges across all 300 facilities. By replacing fragmented, manual logs with a single, unified environment, the system ensured timely access to complete charge data through automated daily ingestion, eliminating the delays that previously crippled our revenue cycle.

This centralized experience provided real-time visibility into charge status, allowing clinical and billing teams to prioritize high-value work and eliminate backlogs. The streamlined process fortified our financial controls by enabling instant issue identification and providing a robust audit trail for every transaction. Furthermore, executive dashboards delivered the actionable insights needed to hold departments accountable and proactively close revenue gaps.
Drastic Reduction in Revenue Leakage: All monthly transactions were captured within the 24-hour window.
Enhanced Audit Readiness: Permanent audit trail across all 300 sites.
System-Wide Accountability: Real-time executive dashboards, empowering leadership to identify and remediate regional performance gaps before they impacted the P&L.
The shift from a manual, chaotic process to a centralized, automated platform has had a profound impact on our health system.
| Reduced Effort with Improved User: | Simplified daily workflows through intuitive, role-based dashboards, which eliminated manual tracking and fragmented processes. |
| Greater Accountability and Collaboration: |
Established clear ownership of charge reviews and standardized workflows with notes, flags, and audit logs to support seamless. |
| Better Decisions with Confidence in Data: |
Provided real-time, accurate, and auditable insights, which empowered teams to proactively resolve issues and make informed decisions. |
